Skin Cancer and Autoimmunity
As Autoimmune Sisters, there are certain groups we are more likely to fall into than the average woman. Like knowing which phlebotomist is the “good” one, which compression socks and gloves actually work, and which current Netflix series is the best to binge on flare days. Unfortunately, our fabulous conditions also puts us at a higher risk to join other groups, like skin cancer.
May is Skin Cancer Awareness Month so skin cancer and autoimmunity feels like an obvious area we need to explore. My own experience with a skin cancer scare two years ago led me to learn that individuals with autoimmune disease are more likely than the general public to be diagnosed with skin cancer [1]. Prior to that, I had no idea of any connection.
The links between skin cancer and autoimmune disease are only more recently coming to the forefront. The causation for why this happens isn’t well established, but two likely reasons make sense and are worth further exploration.
Weakened Immune System
Autoimmune conditions and symptoms are driven by chronic inflammation in the body. [2]
Chronic inflammation on its own weakens the immune system. Add the stress of an autoimmune disease to the mix, and hello inflammation on steroids (see what I did there). A weakened immune system is not as effective as a healthy immune system at detecting when cells start to mutate, as they do in the beginning stages of cancer. The body’s ability to correct the changing cells may be also be diminished. This makes sense when taking into consideration our immune systems are so busy putting out the fires they are detecting in the rest of our bodies. Through all the smoke, visibility and recognization is impaired.
There is also a possible higher risk of skin cancer depending on the type of autoimmune condition you have. Psoriasis and scleroderma, two conditions which present in the skin, “may plausibly cause DNA damage that could promote development of skin cancer.” [3]
Immunocompromising Meds
Not only are our compromised immune systems overly taxed just dealing with the autoimmune disease, but medications are then added to the mix. The medications doctors prescribe to treat autoimmunity, by very definition, suppress the immune system. It’s sort of a double whammy. Medications work to decrease symptoms and prevent new ones from developing by preventing inflammation and stopping the immune system from attacking healthy body tissue [1]. But in doing so, they lower our immune system’s function. Hence decreasing the immune system’s ability to recognize other potential problems, like cancer.
Until a year and a half ago, I had no idea that women with autoimmune disease were more prone to skin cancer. I only learned this after having a skin cancer scare of my own in September 2020.
My Skin Cancer Scare
In August 2020, I went to the dermatologist for my annual visit. I make a point to go annually because living in Florida my entire life and being a fair skinned, blonde haired, blue eyed kiddo, I got burned a lot. I was also a big ole dummy and went to tanning beds in my late teens and early twenties. Do you remember those weird little goggles and tanning stickers? What the heck were we doing?!
At that appointment my doctor biopsied a mole on chest. The September visit was to find out the results of the biopsy testing, which were “slightly abnormal.” My doctor reexamined the area the mole had been removed from and was satisfied that nothing further needed to be done.
Before I left I asked her to take a look at a what I though was a large, light colored freckle on my neck, just below my chin line, that I had recently noticed. In fact I only asked her to check because during this visit she said new spots (moles and freckles) should not appear after about age 35. She checked it out, told me it was actually a mole, and while it didn’t look abnormal, she was going to remove it for biopsy since it had only recently shown up.
The following week I got the results back. “The mole was severely abnormal. You need to make an appointment to come back in to remove a little more of the skin surrounding the mole to make sure they got it all.”
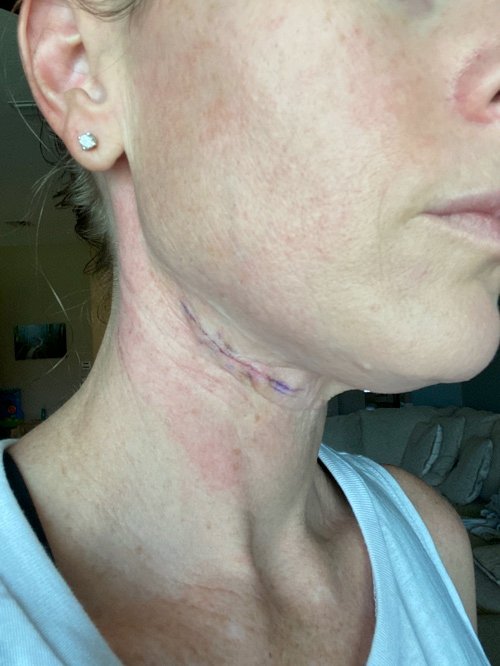
Two weeks after having a “freckle” removed, I was having surgery on my neck. Yes. Outpatient surgery. My dermatologist explained to me that while the lab couldn’t diagnose the mole as melanoma, is was so abnormal that it could have been in the very early stages of melanoma and the skin tested wasn’t enough for a diagnosis of cancer. “But we caught it in time and we’re going to get anything else now,” she confidently stated as my stomach dropped. I’d gone from having a new “freckle” looked at a few weeks prior, to hearing cancer dropped into conversation as we discussed this same “freckle.” I left with a three inch long scar, but clear of any other possible abnormal cells.
I’m the type to do deep dive searches of all things that peek my interest or directly effect me. So you better believe I rabbit holed into the research after this. Here are a few things I can offer as advice so you can avoid a similar situation, or worse.
Tips for Avoiding Skin Cancer
Sunscreen
Sunscreen is important if you’re trying to avoid skin cancer, but the type of sunscreen you use is super important. Be sure you are using mineral, or physical, sunscreen and not chemical sunscreens. Chemical sunscreens are the most widely available sunscreens. However, many companies have recognized the importance of mineral sunscreens and are making more options. You can check out the article I wrote last year for a more in-depth explanation on the difference between mineral and chemical sunscreens. It lists some great mineral sunscreen brand options. Jenn Malecha wrote a great piece on her experience with skin cancer and sunscreen tips. I highly recommend you read it too.
Get Some Sun
While you definitely don’t want to be out in the sun all day long with no protection, some unexposed sun is critical for good health. Aim for 20 minutes of unfiltered (no sunscreen) a day to optimize vitamin D, hormone and mitochondria function. Mutations in the mitochondria, the powerhouse of your cells, have been associated with cancer. [4]
Annual Check Ups with Your Dermatologist
Going to the skin doctor at least once a year is crucial for catching skin abnormalities. Dermatologists are trained to find potential problems and their expertise could save your skin. Literally. If you have a history of abnormal biopsy results, it is recommended you see the dermatologist every six months. If anything new or unusual pops up between checkups, get in a soon as you can and don’t wait until the next scheduled visit. Trust me, it is always better to deal with it sooner rather than later.
Made in the Shade
Avoid being outdoors in direct sunlight during peek sun hours. If you must be outside for long stretches of time, find some shade. Or create your own. Large brimmed hats, long sleeved shirts and sunglasses are always good to have on hand.
No Tanning Beds
I briefly mentioned them earlier, but seriously. They are so bad for you! The direct UV (ultraviolet) light exposure is peak sunlight on steroids. It’s radiation, so keep in mind what that could be doing with every 10 minute session you have (or had).
Know Your Family History
Do you have a family history of melanoma? If so, be extra vigilant about the steps you take to protect yourself from skin cancer because melanoma may have a hereditary link. “About one in every 10 patients diagnosed with melanoma has a family member with a history of the disease. If one or more close biological relatives – parents, brothers, sisters or children – had melanoma, you are at increased risk.” [4]
You’ve Got This
While some of this information may be a shock to you, I hope you find it more empowering than you do scary. Know there are steps you can take to lessen your chances of dealing with skin cancer. Be more aware of and intentional with your approach to the sun. And remember, just because there is a higher risk of skin cancer for us autoimmune warriors, it does not mean skin cancer is inevitable, or even probable. Cue The More You Know rainbow and use this information to have a happier and safer summer!
*The information contained within this article is not meant to treat or diagnose and should not be seen as medical advice. The information is meant to educate. Please consult with a doctor, nutritionist or medical professional for any medical needs and/or questions.*









